Volume 27, Number 1
Melike Aydemir Arslan*, Asiye Ata, and Sevda Kucuk
Ataturk University, Turkey; *Corresponding Author
Given the growing demand for flexible and accessible health education, massive open online courses (MOOCs) have been recognized as instrumental in expanding undergraduate learning. This systematic review was conducted to investigate the use of MOOCs in undergraduate health education, focusing on publication trends, geographic distribution, and key research variables. A total of 31 peer-reviewed articles were reviewed, and data were sourced from six international databases: Web of Science, Scopus, ERIC, EBSCOHost, ScienceDirect, and PubMed. It was found that MOOCs have been integrated into undergraduate health education since 2014, with a notable increase in publications observed after 2022. The highest number of studies was published in China. Student satisfaction was identified as the most frequently studied variable, and medical education was reported as the dominant field. Quantitative research were predominantly used, with sample sizes between 101 and 300 participants. Questionnaires were commonly employed as a data collection tool, and many studies were based on custom-developed MOOCs for their research. Courses were typically between 4 and 6 weeks duration. Improved clinical skills were frequently reported as outcomes, while the lack of practical experience in MOOC-based learning was identified as a major limitation. More practice-oriented teaching approaches were recommended by most studies. To enhance the effectiveness of MOOCs in health education, more innovative and practical implementation strategies are needed. Future research is encouraged to address these gaps and strengthen the impact of MOOCs on undergraduate health programs. The growing role of MOOCs in health education is highlighted, particularly the need to integrate practical components for greater educational impact.
Keywords: MOOCs, undergraduate health education, medical education, systematic review, educational evaluation, clinical skills
In recent years, digitization and opportunities created by information and communication technologies have brought about transformative changes for learners and teachers. With the widespread use of e-learning, systems for both synchronous and asynchronous education have been developed; text materials have been supplemented by audio, animation, and video. Massive open online courses (MOOCs), whose popularity has increased rapidly in recent years, are now an important tool and environment for higher education (Zhu et al. 2018).
For more than two decades, MOOCs have played a key role in the rise of education supported by information and communication technologies, and have been considered a revolutionary development in the field. Open access and scalability are the main principles of MOOCs. Open access refers to courses that are open to anyone who wants to learn and generally refers to being free online. Scalability refers to the fact that courses are designed to support a large number of participants and respond to individual applications (Yuan & Powell, 2013). MOOCs have three main features: (a) they are generally free to use, (b) they provide high-quality education on a variety of subjects, and (c) they are pioneers in lifelong learning. Students have opportunities to learn without any prerequisites or time and space limitations. Thus, it can be said that MOOCs are one of the biggest supporters of lifelong learning (Goh et al., 2017).
MOOCs are widely used in many fields, such as computer science, teaching, engineering, politics, economics, and communication sciences, as well as health studies, especially medical education. In health education, MOOCs have been most common in nursing, pharmacy, and medicine. They have been used to support medical training and interprofessional learning, especially during the COVID-19 pandemic (Dedeilia et al., 2020).
The use of MOOCs in medical education has been seen as an important step towards improving health services (Pouladi et al., 2023). Including perspectives from developing countries can enhance the global relevance of MOOCs, as they have offered scalable and cost-effective solutions in resource-limited settings. However, contextual barriers such as language, technology access, and cultural differences should also be considered (Barteit et al., 2019). MOOCs offer exciting opportunities for learners on a global scale. Carefully selected and collaboratively designed MOOCs can provide nearly unlimited access to undergraduate and postgraduate health education research, and studies examining MOOCs have helped fill knowledge gaps by employing various research models (Setia et al., 2019). The literature has highlighted the effectiveness of e-learning in health education, enhancing knowledge, skills, and satisfaction. Systematic reviews have explored its applications in postgraduate medical education (de Leeuw et al., 2019; Hopcan et al., 2024), low- and middle-income countries (Barteit et al., 2020), and among nurses and medical students (Delungahawatta et al., 2022; Lahti et al., 2014). Common findings have emphasized the importance of well-designed interventions tailored to learners’ needs (Naciri et al., 2021; Regmi & Jones, 2020).
However, despite these advancements, important research gaps remain, particularly in the context of undergraduate health education. Most existing studies focused on postgraduate levels (Nieder et al., 2022; Rowe et al., 2019). As a result, the role of MOOCs in supporting practical, hands-on training at the undergraduate level remains underexplored. This is a significant limitation, as clinical and applied experiences are essential components of health education. However, current MOOC implementations often lack strong frameworks for simulating or supporting real-world practice. These include areas such as patient interaction, procedural training, and interprofessional collaboration. Recent evidence as shown that MOOCs can enhance medical knowledge and clinical skills. In some cases, they even outperform traditional teaching methods (Gao et al., 2021; Yang et al., 2023). Nevertheless, further research is needed to evaluate their effectiveness in delivering comprehensive, practice-oriented education at the undergraduate level.
Despite the growing popularity of MOOCs, their use and efficacy in undergraduate health education remain underexplored. This study aimed to address this gap by conducting a comprehensive systematic review focused on MOOCs in undergraduate health education. It analyzed publication trends, methodologies, key variables, and MOOC characteristics. By bridging this gap, the study provided valuable insights to guide future research and practical applications, shaping the role of MOOCs in meeting the needs of educators and students. The following research questions guided this study.
The purpose of this systematic review was to examine the role of MOOCs in undergraduate health education. The concept of MOOCs in this study was based on definitions widely accepted in the relevant literature. While some studies involved small rather than massive sample groups, this was mostly due to methodological limitations, and these courses still fulfilled the core principles of MOOCs—open access, online delivery, and scalability. Our systematic review was an explicitly and systematically conducted literature review that answered specific questions through the application of a replicable search strategy, with studies included or excluded based on explicit criteria (Gough et al., 2017). Following the identification of potential studies, we applied the PRISMA guidelines (Moher et al., 2015) to ensure a consistent and transparent review process.
This systematic review targeted peer-reviewed articles in English, focusing on the use of MOOCs in undergraduate health education, and indexed in six international databases: Web of Science, Scopus, ERIC, EBSCOHost, ScienceDirect, and PubMed. The search was conducted without any time limitations. The search was undertaken in April 2024. The search strings were (“medical education” OR “health education” OR “nurse education”) AND (“MOOC” OR “massive open online course”). Table 1 summarizes the search strategy for each database.
Table 1
Search Strategies According to Database
| Database | Search strategy |
| WOS | TOPIC=[(“medical education” OR “health education” OR “nurse education”) AND ((“MOOC”) OR “massive open online course”)] |
| ERIC | (“medical education” OR “health education” OR “nurse education”) AND (“MOOC” OR “massive open online course”) |
| SCOPUS | TITLE-ABS-KEY [(“health education” OR “medical education” OR “nurse education”) AND (“MOOC” OR “massive open online course”)] |
| Science Direct | Title, abstract, keywords: (“medical education” OR “health education” OR “nurse education”) AND (“MOOC” OR “massive open online course”) |
| EbscoHost | KW TI AB (medical education or health education or nurse education) AND KW TI AB (mooc or massive open online courses) |
| PubMed | (“medical education”[Title/Abstract] OR “health education”[Title/Abstract] OR “nurse education”[Title/Abstract]) AND (“MOOC”[Title/Abstract] OR “massive open online course”[Title/Abstract]) |
In the initial search, we identified 611 records. After removing 314 duplicates, we used Web-based review software to facilitate data extraction and analysis. The final selection process involved a thorough screening to ensure that studies specifically addressing the applications of MOOCs in undergraduate health education were included (Table 2).
Table 2
Inclusion and Exclusion Criteria
| Inclusion criteria | Exclusion criteria |
| Studies published up to April 2024 | - |
| Journal articles | Book, book chapters, conference papers, dissertations, editorials |
| Application of MOOC in health education | Not about MOOC in health education |
| English language | Not English language |
| Undergraduate education | Graduate education, professional education, public education Full text inaccessible |
The selection of articles to be included in the review was based on a two-dimensional evaluation approach (Vissenberg et al., 2022). The first dimension, methodological trustworthiness, involved assessing the studies according to criteria such as design, context, sampling, data collection, data analysis, and claims and evidence. The second dimension, relevance to the review, focused on evaluating the extent to which each study aligned with the subject matter of the review (Vissenberg et al., 2022). Each study was rated as low, medium, or high based on these criteria (Table 3).
Table 3
Checklist Quality Assessment
| Quality dimension | Criteria | Considerations |
| Methodological trustworthiness | Design | Is the study design appropriate and rigorous? |
| Context | Is the study context clearly described? | |
| Sampling | Is the sampling strategy clearly appropriate? | |
| Data collection | Are data collection methods clearly appropriate? | |
| Data analysis | Is the data analysis clearly appropriate? | |
| Claims/Evidence | Are claims supported by sufficient evidence? | |
| Relevance to review | Does the study directly address key concepts relevant to the review’s objectives? |
Table 4 presents the quality assessment results for the selected studies. A structured rating system was employed based on the two key dimensions of methodological trustworthiness and relevance to the review. Each study was independently evaluated against these dimensions and rated for quality as high (i.e., met both criteria at a high level), medium (i.e., demonstrated moderate alignment) or low (i.e., clear methodological or relevance-related limitations). This classification enabled a more transparent and consistent comparison of the strengths and applicability of the evidence presented. Details are given in Table 4.
Table 4
Quality Assessment on the Selected Studies
| Article title | Methodological trustworthiness | Relevance to the review |
| Delivering a medical school elective with massive open online course (MOOC) | High | High |
| Comparison of the influence of massive open online courses and traditional teaching methods in medical education in China: A meta-analysis | High | High |
| Uncovering motivation and self-regulated learning skills in integrated medical MOOC learning: A mixed methods research protocol | Medium | Medium |
| The Integration of an anatomy massive open online course (MOOC) into a medical anatomy curriculum | High | High |
| Use of H5P interactive learning content in a self-paced MOOC for learning activity preferences and acceptance in an Indonesian medical elective module | Medium | Medium |
| Assessing the effectiveness of massive open online courses on improving clinical skills in medical education in China: A meta-analysis | High | High |
| Creating a ‘choose your topic’ massive open online course: An innovative and flexible approach to delivering injury prevention education | Low | Low |
| Application of online teaching mode combining case studies and the MOOC platform in obstetrics and gynecology probation teaching | Medium | Medium |
| Designing a cassive open online Course (MOOC) in face-to-face sessions. A blended design to teach practical histology | High | High |
| The distance teaching practice of combined mode of massive open online course micro-video for interns in emergency department during the COVID-19 epidemic period | High | High |
| Science education regarding oral health: General health for nonmedical undergraduates applying a SPOC teaching model | Medium | Medium |
| The efficacy of the “Talk-to-Me” suicide prevention and mental health education program for tertiary students: A crossover randomised control trial | High | High |
| Understanding the utility of ‘Talk-to-Me’ an online suicide prevention program | Medium | Medium |
| Effect on exam performance through massive open online courses versus face-to-face classrooms among Indian medical students: An analytic study | High | High |
| Application of a new multi-element integrated teaching mode based on bite-sized teaching, flipped classroom, and MOOC in clinical teaching of obstetrics and gynaecology | High | High |
| Improving undergraduate education of occupational health and occupational medicine applying massive open online courses & problem-based learning | Medium | Medium |
| The ‘Talk-to-Me’ MOOC intervention for suicide prevention and mental health education among tertiary students: Protocol of a multi-site cross-over randomised controlled trial | High | High |
| Teaching effects of the online and offline flipped classroom model (FCM) in the post-epidemic era: Development and feasibility study | Medium | Medium |
| Preventing chronic pain: A human systems approach—Results from a massive open online course | Medium | Medium |
| Health care professionals from developing countries report educational benefits after an online diabetes course | High | High |
| Perception and use of massive open online courses among medical students in a developing country: Multicentre cross-sectional study | Medium | Medium |
| A massive open online course for teaching physiotherapy students and physiotherapists about spinal cord injuries | High | High |
| MOOCs, an innovative alternative to teach first aid and emergency treatment: A practical study | Medium | Medium |
| Implications of a new form of online education | Low | Low |
| The comparison of teaching efficiency between massive open online courses and traditional courses in medicine education: A systematic review and meta-analysis | Medium | Medium |
| A test of the first course (Emergency Medicine) that is globally available for credit and for free | High | High |
| Behavior analysis and formative assessments in online oral medicine education during the COVID-19 pandemic | Medium | Medium |
| Considering the use of massive open online courses (MOOCs) in medical education | Medium | Medium |
| Cyberincivility in the massive open online course learning environment: Data-mining study | Low | Low |
| Delivering an online course in emergency nursing education during the pandemic: What are the effects on students’ learning? | High | High |
| MOOCs and medical education: Hope or hype? | Medium | Medium |
The screening process involved a team of two coders to evaluate 611 titles and abstracts. During this initial screening stage, sensitivity was prioritized over specificity, meaning that papers were more likely to be included than excluded. To reach a consensus, the reasons for inclusion and exclusion were discussed for the first 40 articles at regular meetings. Subsequently, articles were allocated randomly and reviewed based on predefined inclusion and exclusion criteria.
A third researcher randomly reviewed 50 of the articles to ensure consistency and accuracy in coding decisions. Inter-rater reliability was determined using Cohen’s kappa (κ; Cohen, 1960), which measures the degree of consistency among raters. Kappa values are characterized as fair (.40 to . 60), good (.60 to. 75), and excellent (over .75; Bakeman & Gottman, 1997). In our study, the inter-rater reliability was calculated as κ = 1, indicating excellent agreement among the coders.
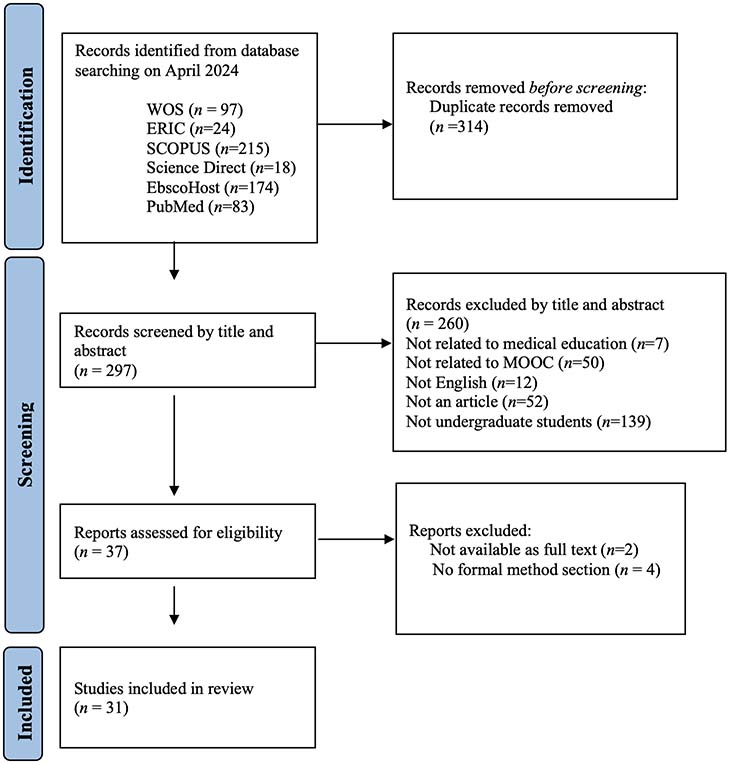
After the initial screening, 351 articles were excluded because they were not (a) related to health education, (b) focused on MOOCs, (c) written in English, (d) journal articles, or (e) centered on undergraduate students. This process left us with 37 reports for full-text assessment. Of these, six reports were excluded because two could not be accessed in full text, and four lacked a formal method section. Consequently, 31 studies were included in the final review for synthesis (Figure 1).
ARRefMan software was used to systematically analyse each study. We created a detailed form designed to capture various aspects of the studies based on our research questions. For the method section analysis, we used the Educational Technology Paper Classification Form developed by Kucuk et al. (2013). This classification helped categorize the studies based on their methodological approaches, allowing for more structured and systematic analysis.
Our systematic review on the use of MOOCs in undergraduate health education analyzed publication trends, including publication year, country of origin, and key variables investigated. We examined the topics covered and research methodologies, along with sample characteristics, sample sizes, and data collection tools. We also identified MOOC platforms and targeted courses. Learning materials and assessment systems were documented. Key implications highlighted the strengths, weaknesses, and suggestions for future research and practice. To identify the strengths and weaknesses of the studies, two researchers independently performed thematic coding by reviewing relevant textual content. Statements were then categorized and grouped through consensus, and recurring themes were extracted to ensure consistency and transparency.
Figure 1
PRISMA Flow Chart

The research findings were analyzed under seven headings based on the research questions. The findings obtained for each question are presented below.
We analyzed the distribution of year of publication for the articles on using MOOCs in undergraduate health education. Since there were no publications before 2014 and the scope of our study was limited to until April 2024, the year 2024 was not included. The distribution of publications between 2014 and 2023 is shown in Figure 2.
Figure 2
Distribution by Year of Publication
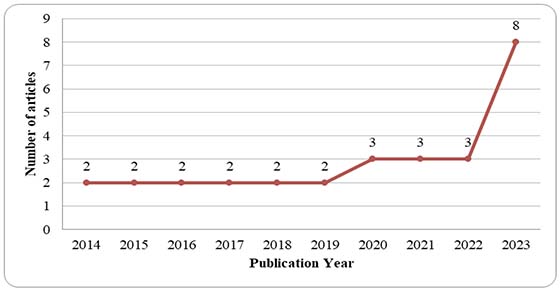
When the distribution of publications by year was examined, it was found that MOOCs have been used in undergraduate health education since 2014. There were two publications between 2014 and 2019. After 2022, a significant increase in the number of publications was observed, with the highest number of publications in 2023 (n = 8). As of April 2024, two publications were identified.
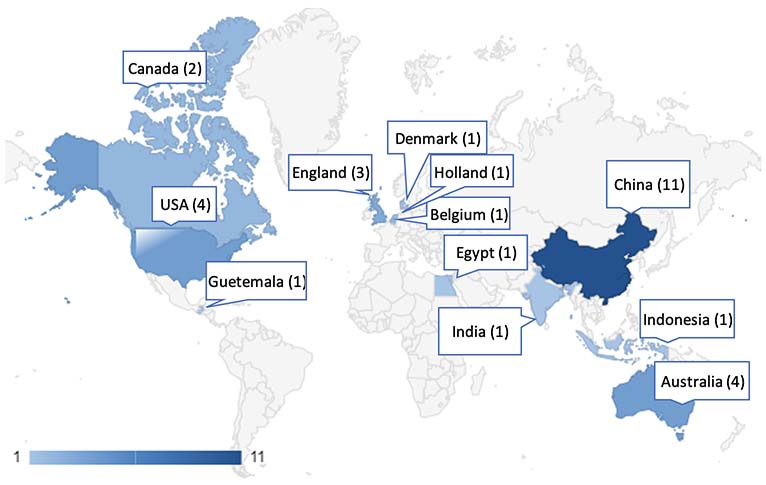
Figure 3 presents a heat map that illustrates the distribution of publications examining the use of MOOCs in undergraduate health education by country. The countries were determined based on the country of the corresponding author. In the studies on using MOOCs in health education, China (n = 11) had the highest number of publications.
Figure 3
Distribution of Publications by Country
The research topics of the studies were identified and are presented in Table 5. A total of 19 different research topics were identified. The research topics were categorized based on the primary focus areas explicitly stated in each study, such as clinical skills, oral health, or public health, under the broader scope of undergraduate medical education. Medical education in general (n = 5) was the most common research topic, followed by emergency nursing/nursing (n = 3), and suicide prevention and mental health education (n = 3).
Table 5
Research Topic
| Research topic | n |
| Medical education | 5 |
| Emergency nursing/nursing | 3 |
| Suicide prevention and mental health education | 3 |
| General internal medicine | 2 |
| Anatomy | 2 |
| Emergency medicine | 2 |
| Obstetrics and gynecology | 2 |
| Oral health, dentistry | 2 |
| Herbal medicine | 1 |
| Injury prevention | 1 |
| Practical histology | 1 |
| Business of medicine | 1 |
| Chronic pain | 1 |
| Cyber incivility | 1 |
| General health | 1 |
| Medical genetics education | 1 |
| Occupational health/ medicine | 1 |
| Diabetes | 1 |
| Physiotherapy | 1 |
The variables used in publications on using MOOCs in undergraduate health education were examined, and their distribution is presented in Figure 4. We found that 23 different variables were used in the studies. The most analyzed variable was satisfaction (n = 17), followed by performance (n = 8).
Figure 4
Distribution of Variables Used in Articles
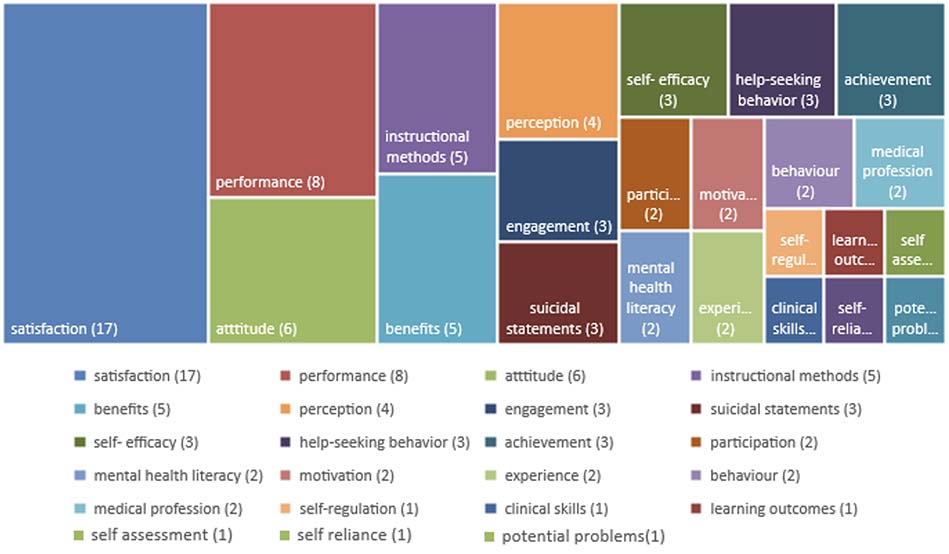
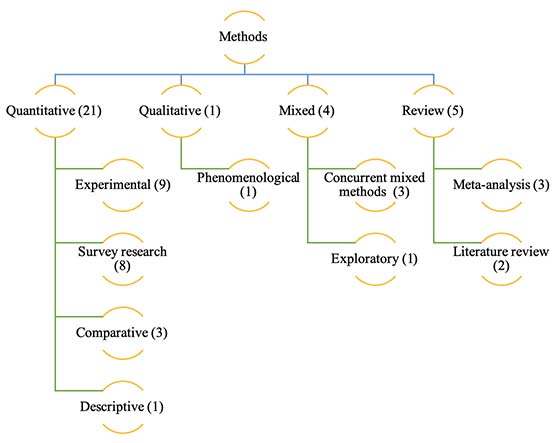
The research methods used in the studies were identified; their distribution is shown in Figure 5. Quantitative methods (n = 21) were the most commonly used in studies on using MOOCs in health education, followed by reviews (n = 5) and mixed methods (n = 4).
Figure 5
Research Methods
The sample populations and sample sizes of the studies were analyzed and are presented in the cross table (Table 6). Due to the focus of our study, samples from the medical field were studied most often (n = 23), followed by samples from the non-medical field (n = 6), nursing (n = 4), and other health fields (n = 2). Most studies were conducted with a sample size between 101 and 300 (n = 12).
Table 6
Distribution of Sample Sizes by Type of Sample Population
| Population | Sample size | |||||||
| 1–10 | 11–30 | 31–100 | 101–300 | 301–1,000 | 1,000+ | Unspecified | Total | |
| Medical | 1 | 1 | 5 | 6 | 6 | 3 | 1 | 23 |
| Non-medical | 1 | 4 | 1 | 6 | ||||
| Nursing | 3 | 1 | 4 | |||||
| Other health | 2 | 2 | ||||||
| Biomedical | 1 | 1 | ||||||
| Dentistry | 1 | 1 | ||||||
| Physiotherapy | 1 | 1 | ||||||
| Total | 1 | 1 | 9 | 12 | 8 | 5 | 2 | |
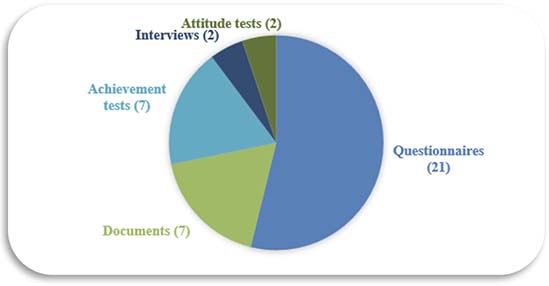
The data collection tools used in the analyzed studies were examined, and the results are presented in Figure 6. Questionnaires (n = 21) were used the most frequently, followed by documents (n = 7) and achievement tests (n = 7). Interviews (n = 2) and attitude, perception, personality, and aptitude tests (n = 2) were the least used.
Figure 6
Data Collection Tools
We examined the use of MOOC to explore how differences in platform design and functionality (e.g., user interface, content delivery methods, learner support features) influenced the pedagogical effectiveness and accessibility of MOOCs in undergraduate health education. MOOC platforms used in the field of health were analyzed (see Table 7). In most studies, MOOCs specifically developed for the study (n = 8) were used. Following this, ready-made platforms were used, though the specific platform was not mentioned in some studies (n = 6). Among the ready-made platforms, EdX (n = 4) was the most frequently used.
Table 7
MOOC Platforms Used in Health Education
| MOOC platform | n |
| Specific | 8 |
| Existing but not written | 6 |
| EdX | 4 |
| Coursera | 3 |
| FutureLearn | 3 |
| Udemy | 1 |
| TalkToMe | 1 |
| Udacity | 1 |
| China University MOOC | 1 |
| NextGenU’s | 1 |
| MOOC Medical Neuroscience | 1 |
| Not given | 3 |
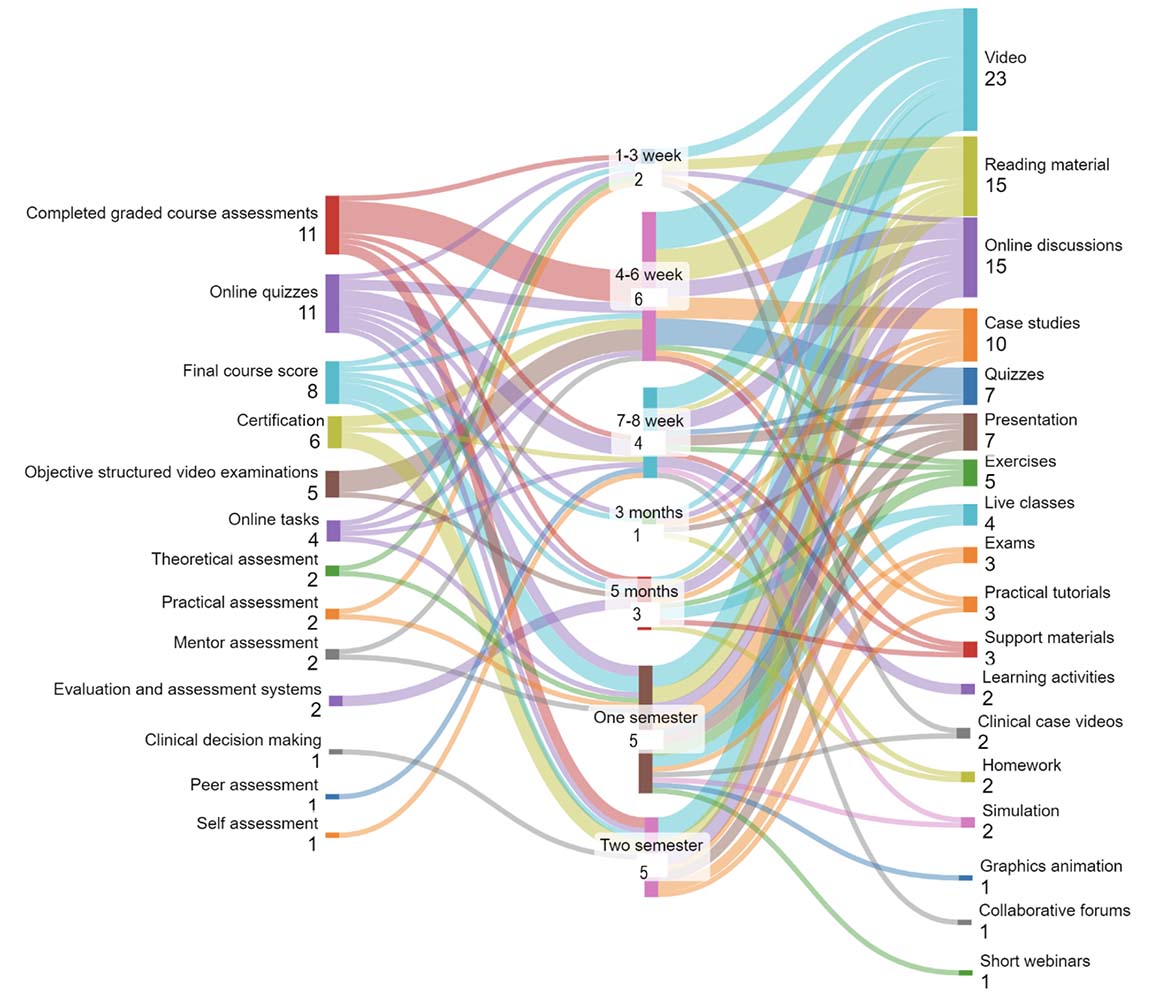
The materials used in MOOCs in health education, assessment types, and MOOC implementation periods were analyzed and are presented in Figure 7. The most common assessment types were completed graded course assessments (n = 11) and online quizzes (n = 11), followed by final course score (n = 8), certification (n = 6), objective structured video examinations (n = 5), and online tasks (n = 4). Theoretical assessment (n = 2), practical assessment (n = 2), mentor assessment (n = 2), and evaluation and assessment systems (n = 2) were used less frequently. Clinical decision-making (n = 1), peer assessment (n = 1), and self-assessment (n = 1) were the assessment types used least.
When the materials used in MOOCs for undergraduate health education were examined, it was found that video (n = 23) was the most preferred. This was followed by reading materials (n = 15), online discussions (n = 15), case studies (n = 10), quizzes (n = 7), presentations (n = 7), exercises (n = 5), live classes (n = 4), exams (n = 3), practical tutorials (n = 3), support materials (n = 3), learning activities (n = 2), clinical case videos (n = 2), homework (n = 2), and simulations (n = 2). The methods used least were graphic animations (n = 1), collaborative forums (n = 1), and short webinars (n = 1).
The most common duration for undergraduate health education MOOCs was between four and six weeks (n = 6), followed by studies conducted over one semester (n = 5) and two semesters (n = 5). Less frequent were studies with a duration of seven to eight weeks (n = 4), five months (n = 3), and one to three weeks (n = 2), respectively. Just one study examined a course of over three months duration (n = 1).
In the one to three week range, video (n = 2) and reading material (n = 2) were the course materials used most often, with different assessment types being used. In the four to six week range, completed graded course assessments (n = 6) and objective structured video examinations (n = 4) were the most common assessment types, while video (n = 7), reading material (n = 6), and quizzes (n = 5) were the materials used most. For courses in the seven to eight week range, online quizzes (n = 3) were the most common assessment type, while video (n = 4) and online discussions (n = 3) were the materials used most. In the three-month range, a range of different assessment types and materials were used equally. In the five-month range, evaluation and assessment systems (n = 2) were the assessments used most, with live classes (n = 2) and online discussions (n = 2) the materials used most. For one semester courses, final course scores (n = 3) and video (n = 4) were used as assessment types and materials, respectively. In the two-semester range, certification (n = 3) and video materials (n = 4) were the most commonly used.
Figure 7
Distribution of the Use of MOOCs in Health Education
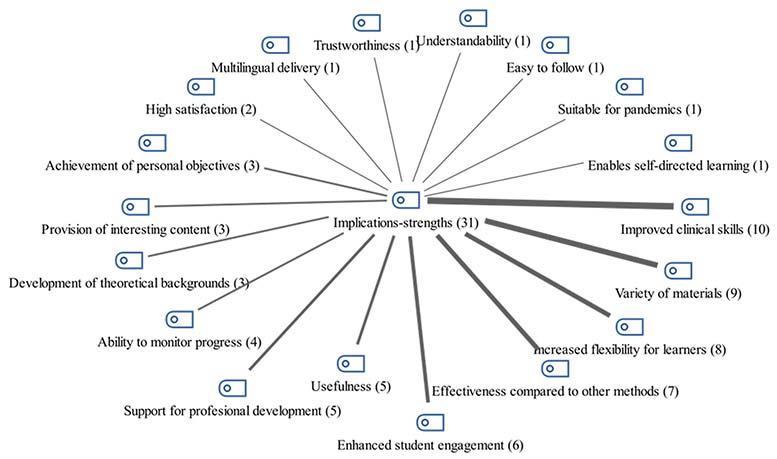
The strengths identified in the use of MOOCs for undergraduate health education were analyzed, and a general distribution was created. The distribution of these strengths is shown in Figure 8. The most common result was improved clinical skills (n = 10). Other positive aspects included variety of materials (n = 9), increased flexibility for learners (n = 8), effectiveness compared to other methods (n = 7), and enhanced student engagement (n = 6). Additional positive results are outlined in Figure 8.
Figure 8
Strengths of Using MOOCs in Health Education
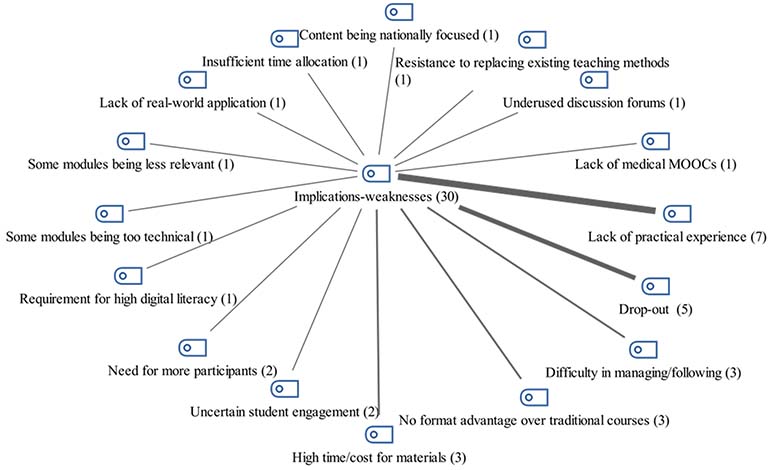
The weaknesses identified in the use of MOOCs for undergraduate health education were also analyzed, and a general distribution was created. The distribution of these weaknesses is shown in Figure 9. The most common weakness was a lack of practical experience (n = 7). Other noted weaknesses included participants' drop-out (n = 5), difficulty in managing/following (n = 3), no format advantage over traditional courses (n = 3), high time/cost for materials (n = 3), uncertain student engagement (n = 2), and need for more participants (n = 2). Additional weaknesses are outlined in Figure 9.
Figure 9
Weaknesses of Using MOOCs in Health Education
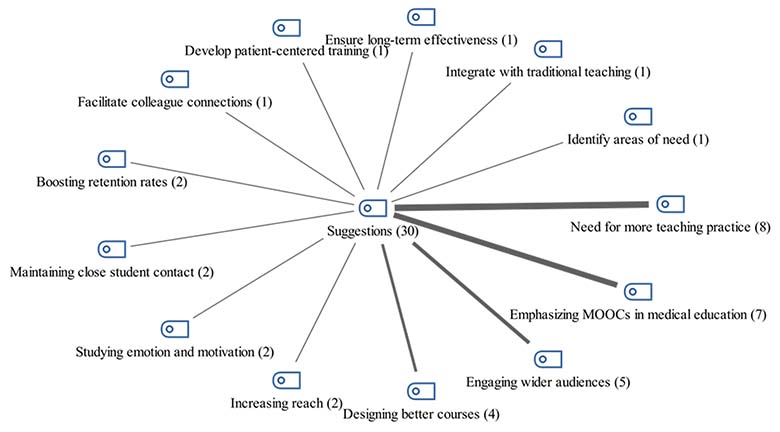
The suggestions in the studies on using MOOCs in health education were analyzed, and a general distribution was created (see Figure 10). The most common suggestion was the need for more teaching practice (n = 8). Other suggestions included emphasizing MOOCs in medical education (n = 7), engaging wider audiences (n = 5), designing better courses (n = 4), increasing reach (n = 2), studying emotion and motivation (n = 2), maintaining close student contact (n = 2), and boosting retention rates (n = 2). Additional suggestions are outlined in Figure 10.
Figure 10
Suggestions for Using MOOCs in Health Education
MOOCs have become a significant tool in medical education, offering a flexible and accessible platform for undergraduate health students, health professionals, and the general public (Longhini et al., 2021; Nieder et al., 2022; Setia et al., 2019). In this study, the place of MOOCs in undergraduate health education has been presented in the context of research methodology, the platform used to host MOOCs and how it is used, and the research results obtained. MOOCs have been used in various fields since 2012, and in undergraduate health education since 2014 (Clark et al., 2017; Liyanagunawardena & Williams, 2014. They have become increasingly popular in online learning in recent years, especially after 2022. The popularity of MOOCs in the medical education field can be explained by the fact that it is a suitable method to support and increase the medical education and interprofessional learning required during COVID-19 (Bettiol et al., 2022; Dedeilia et al., 2020). The upward trend in publications, particularly the sharp increase in 2023, reflected the growing academic interest in leveraging MOOCs for undergraduate health education in the post-pandemic era (Nieder et al., 2022).
While the USA and UK were pioneers in medical MOOCs (Nieder et al., 2022; Rowe et al., 2019), China has emerged as a leader in this field. The first MOOC platform managed by universities in China started in 2013 (Guo, 2014), and medical MOOCs in China have been deeply involved in higher education and seen as important resources (Gong, 2018; Yang et al., 2023). In addition, due to the large population of China, it may be that China has preferred MOOCs for mass education at the undergraduate health education level. The dominance of studies from developed regions highlighted a need for broader geographic inclusion, as contextual differences may significantly influence the effectiveness and design of MOOCs.
When we examined studies of undergraduate health education MOOCs, we determined that satisfaction was the variable studied most often (Gao et al., 2021; Nieder et al., 2022; Rowe et al., 2019; Yang et al., 2023). This trend suggested that researchers prioritized learners’ subjective experiences as a key outcome in evaluating the effectiveness of MOOCs. However, the frequent focus on satisfaction also pointed to a potential gap in assessing deeper learning outcomes such as knowledge retention and skill acquisition, which future studies could explore.
Performance is another key variable; research showed that MOOCs can significantly improve academic performance. A study involving health sciences undergraduates found that those who participated in a MOOC showed better academic performance compared to those who did not (Martín-Valero et al., 2021). Achievement, closely related to performance, has often been measured through course completion and grades. The ability to predict student success in MOOCs and for-credit courses using online interactions has been demonstrated, suggesting that similar factors influence achievement in both contexts (Almeda et al., 2018). Still, it remains unclear whether these performance indicators align with actual skill development in clinical contexts, which has long been a critical consideration in undergraduate health education. Attitude towards MOOCs can affect participation and completion rates, and we found that didactical interventions positively changed learners’ attitudes toward online learning (Khalil & Ebner, 2018). This suggested that pedagogical strategies play a significant role in shaping engagement outcomes. Instructional methods in MOOCs are evolving, with a focus on integrating digital technologies to enhance learning. The post-pandemic shift in health education has highlighted the potential of MOOCs to deliver synchronous and asynchronous learning effectively (Almeda et al., 2018). The benefits of MOOCs, including accessibility and the ability to reach a wide audience, have been demonstrated by the diverse range of health education MOOCs available during the pandemic (Dolores-Maldonado et al., 2021).
The studies we examined focused on a wide range of research topics. Overall, the number of review studies was high. Most of these addressed topics related to medical education, while nursing was the second most studied field. This finding is similar to other studies (Gao et al., 2021; Rowe et al., 2019; Yang et al., 2023).
When the research methods in the studies were analyzed, it was found that mostly quantitative studies were preferred, and among these, experimental studies were the most common research design. Other studies have observed that descriptive/explorative studies (Longhini et al., 2021) and narrative/opinion designs (Rowe et al., 2019) were preferred in research related to medical MOOCs. Survey comparative and descriptive studies were prominent in collecting data from large numbers of students. It was also observed that the number of review studies has increased. This diversity of research methods indicates that different aspects of the use of medical MOOCs continue to be explored. The rapid spread of MOOCs requires continuous use of diverse research methods in order to evaluate their effectiveness and impact on health education outcomes (Bettiol et al., 2022).
In both medical and non-health fields, sample sizes in the range of 101 to 300 are preferred, so studies in the undergraduate health education fields have generally been limited to medium-sized groups. Jordan (2014) stated that despite the high enrolment rates in MOOCs, many students did not complete the course, so sample sizes can be further reduced for effective analyses. More comprehensive analyses may be required to evaluate the effectiveness of MOOCs with a large participant population (Kizilcec & Schneider, 2015). Most of the included studies recruited participants from the medical-related programs, suggesting that MOOCs are more commonly used in medical education than in other health disciplines. The predominance of medical-related samples supports previous studies indicating that the use of MOOCs in medical education has become widespread (Liyanagunawardena & Williams, 2014). The trend toward smaller sample sizes may have reflected feasibility concerns and dropout-related limitations rather than methodological preference, suggesting the need for more diverse and scalable designs in future MOOC research.
Questionnaires were the most commonly used data collection tool in the studies we examined, and this may have been expected because they facilitate the receipt of feedback from participants in online education environments that appeal to large masses, such as MOOCs. Questionnaires enable easy and fast data collection from a large number of participants. In the literature, it was emphasized that questionnaires were frequently used in MOOC research and were ideal for measuring participants’ experiences, satisfaction, and perceptions of learning processes (Longhini et al., 2021; Nieder et al., 2022).
Most of the MOOC platforms used in the field of health were specially developed. Educational needs in the field of health can be very specific, and therefore, general-purpose MOOC platforms may not always be sufficient. Health education requires applied knowledge as well as interdisciplinary skills, so specially designed platforms may be more effective. Among the ready-made MOOCs, EdX, Coursera, and FutureLearn were more preferred. This finding is similar to the studies in the literature (Kononowicz et al., 2015; Longhini et al., 2021)
The analysis of MOOCs in undergraduate health education revealed a variety of materials, assessment types, and implementation times, reflecting the adaptability and potential of MOOCs to enhance learning in this field. MOOCs have become an important tool in health education by offering a wide range of learning resources and assessment methods tailored to different learner needs and contexts (Setia et al., 2019). Various types of assessment have been used in health education MOOCs, with completed graded course assessments and online quizzes the most common. It may be that completed graded course assessments were preferred because they are seen as a criterion in determining the success of MOOCs (Nieder et al., 2022). The variety of assessment types shows that MOOC designers intentionally selected methods that align with the structure and learning objectives of the course (Villarroel et al., 2018).
MOOCs in undergraduate health education have used a variety of materials to facilitate learning. These include lecture videos, interactive discussions, and case studies, which are crucial for engaging learners and enhancing their understanding of complex topics (Alturkistani et al., 2018; Nwameme et al., 2023). Videos have been the most preferred material (Longhini et al., 2021), consistent with the importance of audio-visual learning in online courses (Guo, 2014). High-quality course content and the sharing of educational resources online have been emphasized to improve the learning experience and ensure the accessibility of materials to a broad audience (Cui, 2022).
For MOOCs in undergraduate health education, courses lasting four to six weeks were the most common, which suggested that a medium-duration course was preferred in the field of health. MOOCs are generally planned for short-term and intensive knowledge transfer; flexible and modular approaches are at the forefront of online education (Hew & Cheung, 2014). However, courses spread over one or two semesters were also quite common. Longer courses may be preferred when more comprehensive and in-depth topics need to be addressed. While these findings provide flexibility in online learning, they point to the necessity of longer programs in areas that require intensive knowledge, such as health education (Hauer et al., 2023).
The evaluation types and materials used in MOOCs for health education varied depending on the course duration. While videos and reading materials were generally preferred in short-term MOOCs, more comprehensive evaluation methods and materials were used in long-term courses (Hew & Cheung, 2014). While short-term courses aimed for intensive knowledge transfer, long-term courses allowed students to learn the subject in depth and develop their higher-order skills with a wider variety of materials and assessment methods. This highlighted the flexibility of online education and showed that MOOCs in health education have been structured according to different learning needs (Schettino & Capone, 2022).
The use of MOOCs in undergraduate health education offered several strengths, with the most prominent being the improvement of clinical skills. A meta-analysis conducted in China demonstrated that students participating in MOOC-based courses exhibited improved clinical skill scores (Yang et al., 2023). Other notable benefits have included the provision of diverse materials, increased flexibility for learners, and enhanced student engagement. MOOCs offer a wide range of materials that cater to different learning needs and preferences, which is crucial for health education where diverse content is necessary (Eglseer, 2023). The flexibility of MOOCs allows learners to access content at their own pace and convenience, making it easier for them to balance their studies with other commitments (Eglseer, 2023; Guerrero-Quiñonez et al., 2023; Iniesto et al., 2016). This flexibility is particularly beneficial during unprecedented times, such as the COVID-19 pandemic, where traditional learning methods were disrupted (Rulinawaty et al., 2023). We found that these strengths were distributed across various aspects of learning, contributing to the overall effectiveness of MOOCs in health education.
Analyses of the use of MOOCs in undergraduate health education have revealed several weaknesses. The most frequently cited problem was that online platforms may be insufficient for developing practical skills in health education (Regmi & Jones, 2020). In addition, declining participation revealed that it is difficult to ensure long-term student motivation (Jordan, 2015). Structural weaknesses, such as the difficulty of management and follow-up, as well as the lack of format advantage compared to traditional courses, indicated that MOOCs were inadequate in providing individual feedback while appealing to large audiences. MOOCs cannot fully meet the interaction and practice opportunities offered by face-to-face education (Margaryan et al., 2015). In addition, challenges such as high digital literacy requirements made it difficult for some students to use these platforms effectively due to differences in learners’ digital skills (Kizilcec et al., 2013).
Suggestions for using MOOCs in undergraduate health education have focused on improving both the theoretical and practical aspects of the platforms. The suggestion to provide more teaching practice emphasized the need to support theoretical knowledge with practical applications, and reinforced that practical skills are critical due to the nature of health education (Regmi & Jones, 2020). This reflected a common criticism (Olivares Olivares et al., 2021) that MOOCs may be particularly lacking in terms of developing clinical skills. At the same time, suggestions for greater use of MOOCs in medical education and their appeal to wider audiences imply that the accessibility and impact of these platforms can be increased. Research has shown that MOOCs have the potential to reach more students, especially because they are low-cost and widely accessible (Hollands & Tirthali, 2014; Laurillard & Kennedy, 2017; Liyanagunawardena et al., 2013). To enhance the applicability of these recommendations, integrating hands-on components such as virtual simulations, scenario-based tasks, and peer feedback into MOOC content is essential (Cook et al., 2010; Kononowicz et al., 2015). Additionally, small-scale pilot programs in collaboration with medical institutions could help evaluate the effectiveness and refine practical elements before wider implementation.
Besides this access, course designs need to be improved, which is an important requirement for students to experience more interaction and in-depth learning (Hew & Cheung, 2014). In addition, examining motivational and affective factors may be the key to increasing students’ levels of commitment and engagement in the online learning process (Garrison, 2016).
We systematically analyzed 31 MOOC studies on undergraduate health education from six databases. However, the study had certain limitations that should be acknowledged. First, only English-language publications were included, which may have led to the exclusion of relevant studies published in other languages. Second, the analysis was limited to a specific set of six databases, which may not fully represent all relevant literature in the field. These constraints should be considered when interpreting the findings, as they may affect the generalizability of the results particularly in non-English-speaking or underrepresented regions.
Several implications were revealed. It has been observed that there has been a remarkable increase in the number of studies on undergraduate health education in recent years, especially after the COVID-19 pandemic. Researchers can turn to work in this field. It has been observed that developed countries in the USA, Australia, and Europe, and especially China in Asia, have been active in this field, but there are very few studies in developing countries. Cooperative studies can be carried out with developing countries under the leadership of developed countries. Although many variables were investigated in these studies, the number of studies in which variables specific to medical education were examined was rare. In order to contribute more to the literature on medical education, variables studies less often, yet specific to medical education, could be focused on. We determined that there were more topics on basic medical sciences and general health education and fewer topics on practical skills. MOOCs could incorporate cutting-edge technologies, such as virtual reality, augmented reality, artificial intelligence, and so on, with MOOCs designed for topics that include practical skills.
There were few mixed-method studies in this field. Researchers can contribute to the development of a more comprehensive and in-depth understanding of undergraduate health education by conducting mixed-method studies. In MOOCs for undergraduate health education, data can be collected from a large number of participants and analyzed with machine learning techniques, which allows for individualization of learning processes and in-depth insights to improve educational success. Universities can contribute to a more widespread impact by opening their own MOOCs to other universities and sharing them on other recognized platforms.
In order to support individualized learning in MOOCs, material diversity, course duration, and assessment types may vary according to needs. Increasing the variety of materials, keeping course durations flexible, and using different types of assessment (e.g., self-assessment, peer assessment, practice tests) to support individualized learning in undergraduate health MOOCs can significantly improve student motivation and learning efficiency. Implications based on the literature can be taken into account in future studies. To increase the effectiveness of MOOCs in undergraduate health education, an innovative and holistic approach should be adopted in terms of both content and implementation. Future research could explore the integration of immersive technologies and conduct longitudinal or case-based studies with detailed statistical analyses to assess the long-term effectiveness of MOOCs, particularly in developing practical clinical skills in undergraduate health education.
Almeda, M. V., Zuech, J., Utz, C., Higgins, G., Reynolds, R., & Baker, R. S. (2018). Comparing the factors that predict completion and grades among for-credit and open/MOOC students in online learning. Online Learning, 22(1), 1-18. https://doi.org/10.24059/olj.v22i1.1060
Alturkistani, A., Car, J., Majeed, A., Brindley, D., Wells, G., & Meinert, E. (2018). Determining the effectiveness of a massive open online course in data science for health. In 12th International Conference on e-Learning 2018 (pp. 27-36), Madrid, Spain. https://files.eric.ed.gov/fulltext/ED590297.pdf
Bakeman, R., & Gottman, J. M. (1997). Observing interaction: An introduction to sequential analysis. Cambridge University Press.
Barteit, S., Guzek, D., Jahn, A., Bärnighausen, T., Jorge, M. M., & Neuhann, F. (2020). Evaluation of e-learning for medical education in low-and middle-income countries: A systematic review. Computers & Education, 145, 103726. https://doi.org/10.1016/j.compedu.2019.103726
Barteit, S., Sié, A., Yé, M., Depoux, A., Louis, V. R., & Sauerborn, R. (2019). Lessons learned on teaching a global audience with massive open online courses (MOOCs) on health impacts of climate change: a commentary. Globalization and Health, 15, 1-5. https://doi.org/10.1186/s12992-019-0494-6
Bettiol, S., Psereckis, R., & MacIntyre, K. (2022). A perspective of massive open online courses (MOOCs) and public health. Frontiers in Public Health, 10. https://doi.org/10.3389/fpubh.2022.1058383
Clark, K. R., Vealé, B. L., & Watts, L. K. (2017). A review of the use of massive open online courses (MOOCs) in medical imaging education. Internet Journal of Allied Health Sciences and Practice, 15(2), 1. https://doi.org/10.46743/1540-580X/2017.1659
Cohen, J. (1960). A coefficient of agreement for nominal scales. Educational and Psychological Measurement, 20, 37-46. https://doi.org/10.1177/001316446002000104
Cook, D. A., Levinson, A. J., Garside, S., Dupras, D. M., Erwin, P. J., & Montori, V. M. (2010). Instructional design variations in Internet-based learning for health professions education: A systematic review and meta-analysis. Academic Medicine, 85(5), 909-922. https://doi.org/10.1097/ACM.0b013e3181d6c319
Cui, S. (2022). Analysis and quality improvement research of MOOC. In Proceedings of the 6th International Conference on Digital Technology in Education (pp. 193-199). https://doi.org/10.1145/3568739.3568772
de Leeuw, R., De Soet, A., Van Der Horst, S., Walsh, K., Westerman, M., & Scheele, F. (2019). How we evaluate postgraduate medical e-learning: Systematic review. JMIR Medical Education, 5(1), e13128. https://doi.org/10.2196/13128
Dedeilia, A., Sotiropoulos, M. G., Hanrahan, J., Janga, D., Dedeilias, P., & Sideris, M. (2020). Medical and surgical education challenges and innovations in the COVID-19 era: A systematic review. In Vivo, 34, 1603-1611. https://doi.org/10.21873/INVIVO.11950
Delungahawatta, T., Dunne, S. S., Hyde, S., Halpenny, L., McGrath, D., O’Regan, A., & Dunne, C. P. (2022). Advances in e-learning in undergraduate clinical medicine: A systematic review. BMC Medical Education, 22(1), 711. https://doi.org/10.1186/s12909-022-03773-1
Dolores-Maldonado, G., Cañari-Casaño, J. L., Montero-Romainville, R., & Malaga, G. (2021). Massive open online course (MOOC) opportunities in health education (HE) in a mandatory social isolation context. F1000Research, 10. https://doi.org/10.12688/f1000research.52049.2
Eglseer, D. (2023). Development and evaluation of a massive open online course (MOOC) for healthcare professionals on malnutrition in older adults. Nurse Education Today, 123, 105741. https://doi.org/10.1016/j.nedt.2023.105741
Gao, J., Yang, L., Zou, J., & Fan, X. (2021). Comparison of the influence of massive open online courses and traditional teaching methods in medical education in China: A meta‐analysis. Biochemistry and Molecular Biology Education, 49(4), 639-651. https://doi.org/10.1002/bmb.21523
Garrison, D. R. (2016). E-learning in the 21st century: A community of inquiry framework for research and practice. Routledge. https://doi.org/10.4324/9781315667263
Goh, W., Ayub, E., Wong, S. Y., & Lim, C. L. (2017). The importance of teacher’s presence and engagement in MOOC learning environment: A case study. In 2017 IEEE Conference on e-Learning, e-Management and e-Services (pp. 127-132). https://doi.org/10.1109/IC3e.2017.8409250
Gong, Z. (2018). The development of medical MOOCs in China: Current situation and challenges. Medical Education Online, 23(1), 1527624. https://doi.org/10.1080/10872981.2018.1527624
Gough, D., Oliver, S., & Thomas, J. (2017). An introduction to systematic reviews. Sage.
Guerrero-Quiñonez, A. J., Bedoya-Flores, M. C., Mosquera-Quiñonez, E. F., Ango-Ramos, E. D., & Lara-Tambaco, R. M. (2023). The MOOC as an alternative model for university education. Ibero-American Journal of Education & Society Research, 3(1), 280-286. https://doi.org/10.56183/iberoeds.v3i1.630
Guo, Y. (2014). MOOCs and the future of China’s higher education. Journal of Higher Education Management, 8(5), 29-33. https://doi.org/10.13316/j.cnki.jhem.2014.05.002
Hauer, K. E., Chang, A., van Schaik, S. M., Lucey, C., Cowell, T., & Teherani, A. (2023). It’s all about the trust and building a foundation: Evaluation of a longitudinal medical student coaching program. Teaching and Learning in Medicine, 35(5), 550-564. https://doi.org/10.1080/10401334.2022.2111570
Hew, K. F., & Cheung, W. S. (2014). Students’ and instructors’ use of massive open online courses (MOOCs): Motivations and challenges. Educational Research Review, 12, 45-58. https://doi.org/10.1016/j.edurev.2014.05.001
Hollands, F. M., & Tirthali, D. (2014). Why do institutions offer MOOCs? Online Learning, 18(3), n3. http://dx.doi.org/10.24059/olj.v18i3.464
Hopcan, S., Polat, E., & Albayrak, E. (2024). Research trends in e-learning practices for postgraduate medical education: A systematic review. Education and Information Technologies, 29(5), 5921-5945. https://doi.org/10.1007/s10639-023-12035-6
Iniesto, F., McAndrew, P., Minocha, S., & Coughlan, T. (2016). Accessibility of MOOCs: Understanding the provider perspective. Journal of Interactive Media in Education, 2016(1). https://doi.org/10.5334/jime.430
Jordan, K. (2014). Initial trends in enrolment and completion of massive open online courses. International Review of Research in Open and Distributed Learning, 15(1), 133-160. https://doi.org/10.19173/irrodl.v15i1.1651
Jordan, K. (2015). Massive open online course completion rates revisited: Assessment, length and attrition. International Review of Research in Open and Distributed Learning, 16(3), 341-358. https://doi.org/10.19173/irrodl.v16i3.2112
Khalil, M., & Ebner, M. (2018). Can learning analytics find success in didactical measurements? Results from a MOOC case study. In D. Ifenthaler (Ed.), Digital workplace learning: Bridging formal and informal learning with digital technologies (pp. 211-225). Springer. https://doi.org/10.1007/978-3-319-46215-8_12
Kizilcec, R. F., Pérez-Sanagustín, M., & Maldonado, J. J. (2013). Self-regulated learning strategies predict learner behavior and goal attainment in massive open online courses. Computers & Education, 104, 18-33. https://doi.org/10.1016/j.compedu.2016.10.001
Kizilcec, R. F., & Schneider, E. (2015). Motivation as a lens to understand online learners: Toward data-driven design with the OLEI scale. ACM Transactions on Computer-Human Interaction, 22(2), 1-24. https://doi.org/10.1145/2699735
Kononowicz, A. A., Berman, A. H., Stathakarou, N., McGrath, C., Bartyński, T., Nowakowski, P., Malawski, M., & Zary, N. (2015). Virtual patients in a behavioral medicine massive open online course (MOOC): A case-based analysis of technical capacity and user navigation pathways. JMIR Medical Education, 1(2), e8. https://doi.org/10.2196/mededu.4394
Kucuk, S., Aydemir, M., Yildirim, G., Arpacik, O., & Goktas, Y. (2013). Educational technology research trends in Turkey from 1990 to 2011. Computers & Education, 68, 42-50. https://doi.org/10.1016/j.compedu.2013.04.016
Lahti, M., Hätönen, H., & Välimäki, M. (2014). Impact of e-learning on nurses’ and student nurses knowledge, skills, and satisfaction: A systematic review and meta-analysis. International Journal of Nursing Studies, 51(1), 136-149. https://doi.org/10.1016/j.ijnurstu.2012.12.017
Laurillard, D., & Kennedy, E. (2017). The potential of MOOCs for learning at scale in the Global South. Center for Global Higher Education, 31. http://dx.doi.org/10.5287/ora-gagqxyjje
Liyanagunawardena, T. R., Adams, A. A., & Williams, S. A. (2013). MOOCs: A systematic study of the published literature 2008–2012. The International Review of Research in Open and Distributed Learning, 14(3), 202-227. https://doi.org/10.19173/irrodl.v14i3.1455
Liyanagunawardena, T. R., & Williams, S. A. (2014). Massive open online courses on health and medicine. Journal of Medical Internet Research, 16(8), e191. https://doi.org/10.2196/jmir.3439
Longhini, J., De Colle, B., Rossettini, G., & Palese, A. (2021). What knowledge is available on massive open online courses in nursing and academic healthcare sciences education? A rapid review. Nurse Education Today, 99, 104812. https://doi.org/10.1016/j.nedt.2021.104812
Margaryan, A., Bianco, M., & Littlejohn, A. (2015). Instructional quality of massive open online courses (MOOCs). Computers & Education, 80, 77-83. https://doi.org/10.1016/j.compedu.2014.08.005
Martín-Valero, R., Pastora-Bernal, J. M., Ortiz-Ortigosa, L., Casuso-Holgado, M. J., Pérez-Cabezas, V., & Ruiz-Párraga, G. T. (2021). The usefulness of a massive open online course about postural and technological adaptations to enhance academic performance and empathy in health sciences undergraduates. International Journal of Environmental Research and Public Health, 18(20), 10672. https://doi.org/10.3390/ijerph182010672
Moher, D., Shamseer, L., Clarke, M., Ghersi, D., Liberati, A., Petticrew, M., & Stewart, L. A. (2015). Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Systematic Reviews, 4(1), 1-9. https://doi.org/10.1186/2046-4053-4-1
Naciri, A., Radid, M., Kharbach, A., & Chemsi, G. (2021). E-learning in health professions education during the COVID-19 pandemic: A systematic review. Journal of Educational Evaluation for Health Professions, 18. https://doi.org/10.3352/jeehp.2021.18.27
Nieder, J., Nayna Schwerdtle, P., Sauerborn, R., & Barteit, S. (2022). Massive open online courses for health worker education in low-and middle-income countries: A scoping review. Frontiers in Public Health, 10, 891987. https://doi.org/10.3389/fpubh.2022.891987
Nwameme, A., Dako-Gyeke, P., Asampong, E., Allotey, P., Reidpath, D. D., Certain, E., Vahedi, M., Ross, B., Maher, D., & Launois, P. (2023). Improving understanding of disease control implementation research through a MOOC with participants from low-and middle-income countries: Evaluating participant reactions and learning. PLoS Neglected Tropical Diseases, 17(3), e0011139. https://doi.org/10.1371/journal.pntd.0011139
Olivares Olivares, S. L., Hernández, R. I. E., Corolla, M. L. T., Alvarez, J. P. N., & Sánchez-Mendiola, M. (2021). MOOC learning assessment in clinical settings: Analysis from quality dimensions. Medical Science Educator, 31(2), 447-455. https://doi.org/10.1007/s40670-020-01178-7
Pouladi, E., Yazdi, M. T., Salehi, M., & Moradi, S. (2023). Use of massive online open courses (MOOCs) model in virtual education development in first macro-region universities of medical sciences in countrywide territorial planning. Journal of Education and Health Promotion, 12, 326. https://doi.org/10.4103/jehp.jehp_1221_22
Regmi, K., & Jones, L. (2020). A systematic review of the factors—enablers and barriers—affecting e-learning in health sciences education. BMC Medical Education, 20(1), 1-18. https://doi.org/10.1186/s12909-020-02007-6
Rowe, M., Osadnik, C. R., Pritchard, S., & Maloney, S. (2019). These may not be the courses you are seeking: a systematic review of open online courses in health professions education. BMC Medical Education, 19, 1-11. https://doi.org/10.1186/s12909-019-1774-9
Rulinawaty, R., Priyanto, A., Kuncoro, S., Rahmawaty, D., & Wijaya, A. (2023). Massive open online courses (MOOCs) as catalysts of change in education during unprecedented times: A narrative review. Jurnal Penelitian Pendidikan IPA, 9(Special issue), 53-63. https://doi.org/10.29303/jppipa.v9iSpecialIssue.6697
Schettino, G., & Capone, V. (2022). Learning design strategies in MOOCs for physicians’ training: A scoping review. International Journal of Environmental Research and Public Health, 19(21), 14247. https://doi.org/10.3390/ijerph192114247
Setia, S., Tay, J. C., Chia, Y. C., & Subramaniam, K. (2019). Massive open online courses (MOOCs) for continuing medical education: Why and how? Advances in Medical Education and Practice, 2019(10), 805-812. https://doi.org/10.2147/AMEP.S219104
Villarroel, V., Bloxham, S., Bruna, D., Bruna, C., & Herrera-Seda, C. (2018). Authentic assessment: Creating a blueprint for course design. Assessment & Evaluation in Higher Education, 43(5), 840-854. https://doi.org/10.1080/02602938.2017.1412396
Vissenberg, J., d’Haenens, L., & Livingstone, S. (2022). Digital literacy and online resilience as facilitators of young people’s wellbeing? A systematic review. European Psychologist, 27(2), 76-85. https://doi.org/10.1027/1016-9040/a000478
Yang, L., Zou, J., Gao, J., & Fan, X. (2023). Assessing the effectiveness of massive open online courses on improving clinical skills in medical education in China: A meta-analysis. Heliyon, 9(8), e19263. https://doi.org/10.1016/j.heliyon.2023.e19263
Yuan, L., & Powell, S. (2013). MOOCs and open education: Implications for higher education. CETIS. https://e-space.mmu.ac.uk/619735/
Zhu, M., Sari, A., & Lee, M. M. (2018). A systematic review of research methods and topics of the empirical MOOC literature (2014–2016). The Internet and Higher Education, 37, 31-39. https://doi.org/10.1016/j.iheduc.2018.01.002

MOOCs Reshaping Undergraduate Health Education: A Systematic Review by Melike Aydemir Arslan, Asiye Ata, and Sevda Kucuk is licensed under a Creative Commons Attribution 4.0 International License.